Courtesy of connect.innovateuk.org
The UR Medical Center became the site of the first total artificial heart (TAH) implant in upstate New York on April 4 when surgeons inserted a SynCardia TAH into Gaetano Orlando, 49, a retired Buffalo Sabres and Rochester Amerks hockey player suffering from heart failure.
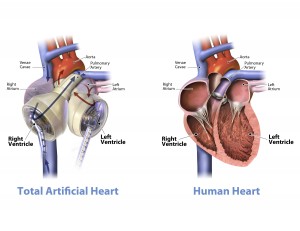
Before the SynCardia TAH, prevailing artificial heart devices required continued assistance from either the heart’s left or right ventricle — the main chambers responsible for pumping blood out to the body. SynCardia’s new device, however, functions largely on its own. Orlando was diagnosed with sarcoidosis, a rare cardiovascular disease that left both his ventricles incapacitated, thereby making him an ideal candidate for the cutting-edge procedure.
Surgeons removed nearly all of Orlando’s heart except for his left and right atria, aorta and pulmonary artery, which were later attached to the implant.
The longest a patient has lived with a SynCardia TAH is 46 months, which, although not a long-term solution, can extend the life of a person with critical heart failure until a permanent transplant is made.
Part of what makes this surgery so remarkable is not only the technology involved but also that URMC is one of only a few hospitals in the nation to have completed the implant, according to Orlando’s cardiologist Eugene Storozynsky.
“I would like to stress that the only other facility [in New York State] where this technology is available is Columbia University in NYC, where doctors have only implanted two of these devices,” he explained. He also cited the fact that URMC is joining the ranks of only 30 locations nationwide offering the procedure.
In order to pump blood through the body, the SynCardia TAH initially entails a vacuum with a 400-pound driver in tow, severely restricting user mobility. Smaller, more portable drivers are ultimately available for patients as they recover from the surgery, allowing them to lead a more normal life despite an almost entirely artificial heart powering their bodies.
“The next frontier is in their miniaturization, to where they may become fully implantable, including the power source, [which would] be recharged externally through the skin,” Storozynsky said. “Once this can occur reliably and successfully, the TAH may then someday replace heart transplantation as an option for patients.”
In addition to Storozynsky’s contribution, the operation was performed by a team from URMC’s Artificial Heart Program, including the program’s surgical director H. Todd Massey and transplant cardiologist Leway Chen.
With 3,100 individuals in the U.S. currently waitlisted for a heart transplant, the odds of being selected for and of surviving the procedure were overwhelmingly against Orlando. Thanks to the work of URMC physicians and the latest in medical technology however, he is alive against all previous odds.
Sklar is a member of the class of 2014.